 I recently wrote an article titled ‘Caesarean section changes during my time as an obstetrician’ in which I mentioned that there had been an increase in the Caesarean section rate over more recent times. One reason for this is that there has been a corresponding decrease in the operative (also called assisted) vaginal delivery rate. Many of the women who would have had operative vaginal deliveries in the past now have Caesarean section deliveries. This has to do with Caesarean sections being now safer than other than straight forward easy operative vaginal deliveries.
I recently wrote an article titled ‘Caesarean section changes during my time as an obstetrician’ in which I mentioned that there had been an increase in the Caesarean section rate over more recent times. One reason for this is that there has been a corresponding decrease in the operative (also called assisted) vaginal delivery rate. Many of the women who would have had operative vaginal deliveries in the past now have Caesarean section deliveries. This has to do with Caesarean sections being now safer than other than straight forward easy operative vaginal deliveries.
When I started my training as an obstetrician I recall a vaginal delivery was preferred to a Caesarean section delivery. Operative vaginal deliveries were done much more frequently than today. There were various reasons for this including…
- In the past vaginal deliveries (including operative vaginal deliveries) were considered safer than Caesarean section deliveries.
- In the past obstetricians were better trained, more skilled and more experienced at doing complicated vaginal deliveries and procedures than they are today. Being better trained and more experienced and skilled increased the safety of operative vaginal deliveries.
- In the past there were many more difficult operative vaginal deliveries than today. That included ‘trial of forceps’ deliveries, where there was a lack of progress in second stage labour and concern about the possibility and safety of a forceps operative vaginal delivery. Today a Caesarean section is preferred to a potentially more difficult operative vaginal delivery which is now recognised to have a greater risk for mother and baby.
- Breech presenting babies were routinely delivered vaginally. Piper forceps were used to facilitate delivery of the baby’s head. It is now recognised a Caesarean section delivery is safer for a baby in a breech presentation.
- There were no concerns about litigation if something went wrong and so doctors did what they thought was appropriate without being concerned about being sued. The incidence of medical litigation when I was a trainee and junior obstetrician was very low. Doctors now practice a more ‘defensive’ medicine whether they tend to choose the option which is less likely to result in litigation, but which may not be necessary.
- Patients in the past usually did not question the doctor’s decision, but accepted the doctor was doing what was best for her and her baby.
When was an operative vaginal delivery done?
The criteria in my time has always been the baby’s head must be engaged in the pelvis. Before my time there were “high forceps’ deliveries (baby’s head not engaged) which were extremely dangerous procedures.
On vaginal examination engagement of baby’s head is determined by the lowest bony part of baby’s head being at least at the level of the ischial spines of the bony pelvis. The ischial spine is a bony landmark felt at the side of the pelvis which is about halfway down the pelvic wall. The head at this level implies the top half of the head is in the pelvis. The lower the baby’s head is in the pelvis the safer the operative vaginal delivery.
For a forceps delivery the women should be in second stage labour (cervix fully dilated). Occasionally forceps are used when there is still a small amount of cervix (called ‘lip of cervix’ ) present.
In the past a vacuum cup was often applied before full dilatation. The literature reports the vacuum cup being used historically even at 4cm cervical dilatation and without engagement of baby’s head. They would have been very dangerous vaginal deliveries but back in those times a vaginal delivery was preferred to Caesarean section delivery.
The indications for an operative vaginal delivery include lack of progress with pushing in second stage, maternal exhaustion, foetal distress or maternal illness where prolonged “bearing down” or pushing efforts would be risky.
‘Lack of progress with pushing’ in the past usually implied a degree of cephalo-pelvic disproportion (baby’s head being too big for the birth canal). These deliveries had to be done carefully and great skill, because to the increased risk to baby and mother. There was the possibility of a ‘failed forceps’ delivery where it was decided it was too tight a fit for a safe vaginal delivery. In this case a Caesarean section was done.
Epidurals were less common in the past, and so there were fewer cases of ‘lack of progress’ in second stage labour due to lack of pushing or ineffective pushing because of an epidural block.
Today, to minimise the need for an operative vaginal delivery because of an epidural, if a labouring woman has an epidural block I prefer a woman not to push (‘active’ second stage) until the baby’s head as descended as low as possible in the pelvis. If there is no foetal distress to have a long ‘passive’ second stage has no risk and increases the likelihood of a spontaneous vaginal delivery or else it will be much easier and safer operative vaginal delivery.
Forceps and Vacuum cups
In my experience in the past forceps operative vaginal deliveries were much more popular than vacuum cup operative vaginal deliveries. In the past almost all my operative vaginal deliveries were done with forceps.
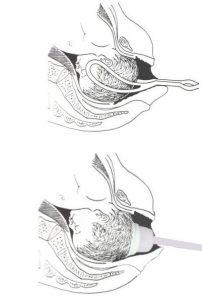
The vacuum cups we use today had not been invented. It was not unusual with other older style of vacuum cup of the past for it to ‘come off’ baby’s head with traction and so vacuum cups were less reliable. In the past the cups (Malmstrom vacuum extractor) were made of metal. There was a choice of shapes. The shape of the cup used was determined on the position of the baby’s head. Cup vacuum was achieved by midwife using a bicycle pump attached indirectly by tubing to the cup.
Success with forceps was predictable, as they never came off the baby’s head. Forceps were always successful in delivery of baby’s head unless the head was found to be too big to the bony birth canal (‘failed forceps’).
The use of forceps has more risk than using a vacuum cup. Because forceps do not come off it was possible to pull too hard and damage the baby with the delivery. I am pleased to report that I have done hundreds of forceps deliveries over many years and have never damaged a baby with their use.
I now prefer to use the vacuum cup to forceps. The cups today are more reliable and are disposable. While I am not worried about damaging baby with forceps, there is usually more maternal trauma than if a vacuum cup is used. There is need, I believe, to always do an episiotomy when using forceps to minimise the risk of significant perineal tearing. That is not the case with vacuum cup. The forceps are placed on the sides of the baby’s head and so increase the stretch of the vaginal entrance with delivery and increase the likelihood of tearing. The vacuum cup is attached to the top of baby’s head and so does not increase the stretching of the vaginal entrance and does not increase the likelihood of perineal tearing.
Today there are only three types of forceps available in the hospitals in which I deliver.
Neville Barnes forceps – used when the baby’s head is in the up-down position. If baby’s face is towards the floor this is called an occipito-anterior position and if baby’s face is towards the ceiling it is called an occipito-posterior position.
Kielland’s forceps – used when baby’s head is not in the up-down position. Kielland’s forceps are used to rotate the head to the up-down position and delivery the head once in that position. The use of Kielland’s forceps is associated with considerable risk for mother and baby and so now, especially with more reliable vacuum cups, a Kielland’s forceps delivery is done infrequently. I believe most junior obstetricians today would not have had adequate exposure in their training to using Kielland’s and so would not have the appropriate level of clinical skill to use Kielland’s forceps safely.
Wrigley’s lift-out forceps – Used when a forceps delivery was needed and baby’s head was at the perineum and when forceps were needed to help with delivery of baby’s head at a Caesarean section delivery. Today they are only used when forceps were needed to help with delivery of baby’s head at a Caesarean section delivery.
In the past I have also used ….
- Simpsons forceps – instead of Neville Barnes Forceps when the baby’s head was in the direct occipito-anterior or direct occipito-posterior position.
- Piper forceps – for facilitating delivery of the after-coming head If a breech vaginal delivery. Piper forceps have long handles and so are safer to use than other forceps in this context.
Anaesthetics for operative vaginal delivery
Operative vaginal deliveries were done with an epidural anaesthetic block, if an epidural was in situ for labour pain relief. If not then then at the time of delivery there was a caudal regional block inserted or a pudendal nerve block with local anaesthetic infiltration of the perineum for the episiotomy. A caudal regional block and pudendal block are not as effective for pain relief as an epidural block and a forceps operative vaginal delivery could be more painful than desired.
Today there is a much higher incidence of epidural blocks than in the past. As well there is usually no need for a regional anaesthetic when using a vacuum cup as there is usually is no more painful than a spontaneous vaginal delivery.
Today
My preference is not to do an operative vaginal delivery. As mentioned above many operative vaginal deliveries related to an epidural can be avoided by having patience and advising the labouring woman not to push (‘active’ second stage) until the baby’s head has descended as low as possible in the pelvis. If there is no foetal distress to have a long ‘passive’ second stage has no risk and increases the likelihood of a spontaneous vaginal delivery or else it will be much easier and safer operative vaginal delivery.
If an operative vaginal delivery is needed today I prefer to use the vacuum cup rather than forceps, as mentioned above. This is because a vacuum cup delivery is usually less traumatic for the mother. With forceps an episiotomy is needed. As well there can be significant tearing. Usually an episiotomy is not needed with a vacuum cup delivery and usually there either no or only minor perineal tearing.
Also see article titled: ‘Vacuum and Forceps’

