 I saw a couple today for follow up after her third miscarriage.
I saw a couple today for follow up after her third miscarriage.
I met her for the first time for her first antenatal visit of this most recent pregnancy. She was nine weeks pregnant by dates at the time of her first antenatal visit. She was well and excited. All was well. There had been no bleeding since her last menstrual period. She had had an ultrasound scan at seven weeks and all appeared good.
She had had had had 2 previous pregnancies which had ended as miscarriages (one was at seven weeks with a curettage of uterus and the other at five weeks and without a curettage of uterus).
She and her husband had been seen by a subfertility subspecialist who had done extensive investigations re recurrent miscarriage prior to this pregnancy and no abnormality was found.
I did an ultrasound scan of her baby at the first antenatal visit. I had to sadly advise her that there had been foetal demise. The baby measures 6 weeks (crown-rump length) and there was no foetal heart motion. They were devastated.
She had suction curettage of uterus done by me. I sent tissue for histology and chromosome studies.
The histology report was degenerate immature products of conception.
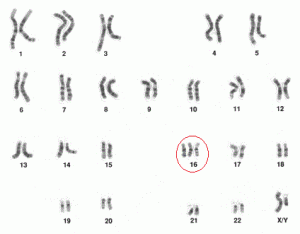
The karyotype was reported 47, XY, +16 or a male conceptus with trisomy 16, which is consistent with spontaneous pregnancy loss, and is the second commonest karyotype cause for miscarriage.
Advising her of the reason for her pregnancy loss was very helpful in closure.
I advised her I have no insight into why she had miscarried the two prior times but this recent miscarriage should be regarded as a ‘one-off’ and have no bearing in the future. She was relieved.
She will start trying again soon.
I advised her that I wanted to see her early in her next pregnancy for close pregnancy monitoring. This was not because of her last pregnancy loss but her previous two. Hopefully all will work out well next time.
Foetal karyotype abnormalities account for at least 60% of first trimester miscarriages. I routinely send products of conception for karyotype studies. I am amazed that the majority of my obstetrician colleagues don’t bother sending miscarriage products of conception for karyotype studies.
I find knowing the reason why a miscarriage has happened helps the grieving couple move on and plan for the future with more confidence. It also helps me in planning appropriate management of the next pregnancy.

