A 23-year-old woman saw me for a gynaecology consultation in the hope I could explain to her what went wrong with her last delivery eight months earlier when she had a ruptured uterus. Also, she wanted my management of abdominal pain she has had since then.
I was very saddened by what she said, and especially knowing that the outcome could have been very different with different management.
 Her story began with her first pregnancy in 2011. An obstetrician whom she saw in the antenatal period advised her that her pelvis would most likely be too small for a vaginal delivery of her large baby. An elective Caesarean section was suggested. She had an elective Caesarean section as a public patient at 38 weeks pregnant. Her baby was born in good condition and weighed four kilograms.
Her story began with her first pregnancy in 2011. An obstetrician whom she saw in the antenatal period advised her that her pelvis would most likely be too small for a vaginal delivery of her large baby. An elective Caesarean section was suggested. She had an elective Caesarean section as a public patient at 38 weeks pregnant. Her baby was born in good condition and weighed four kilograms.
She was managed as a public patient in her next pregnancy at the same public hospital where she had her first delivery. A VBAC (Vaginal Birth After a Caesarean section) attempt was recommended. There was uterine rupture in labour that resulted in a life-threatening risk to her and her baby. Her baby has done well. She has ongoing lower abdominal pain since the delivery, which I suspect is due to scar tissue and possibly adhesions that have formed with healing.
I have managed many women over the years who have had successful VBAC attempts. I have never had a patient who has ruptured her uterus. That does not mean it won’t even happen to me. It does mean I am very careful and I am very conscious of the risk of a ruptured uterus and that I do all possible to minimise this risk and diagnose it early should it occur.
In the past, a VBAC attempt was called a ‘Trial of Scar’ labour. A VBAC attempt labour is a ‘trial’ to see if the uterine scar from the previous Caesarean section remains intact in labour. I consider ‘Trial of Scar’ a better name as everyone is reminded of the risk of the labour after a Caesarean section.
What she told me of her pregnancy and labour management I find very concerning. Aspects of her management were not in accord with RANZCOG guidelines. There may be some inconsistencies with what really happened, as I only have her recollection and the hospital discharge summary for information. I do not have the hospital notes to cross-reference.
Concluding from the information available, I do not believe it was appropriate to advise her to have a VBAC attempt. Rather, she should have had an elective Caesarean section. In labour, her uterus did rupture. It is not possible to know from the information at hand when in her labour this did happened. I believe clinical warnings in labour that rupture was imminent were not recognised or, if recognised, acted on. Also, there was delay in recognising uterine rupture had happened and excessive delay in doing a Caesarean section delivery.
Most of her antenatal visits were with a midwife, and only three were with a doctor. As a high-risk patient, I do not consider this appropriate antenatal care. She should not have attended a midwife’s clinic, which is only suitable for low-risk patients.
She was told by the midwife and the doctor that the obstetrician she had seen antenatally in her first pregnancy ‘was silly’ to recommend a Caesarean section and that she should have a VBAC this time. She was told she was the perfect candidate for a successful VBAC. She said, while she was advised there was a risk of uterine rupture, she was reassured by both the midwife and the doctor that the risk of uterine rupture was very small and that it rarely happened. The implications of uterine rupture for her and her baby were never discussed. She did not have CT pelvimetry to assess if the size and shape of her pelvis were adequate for a vaginal birth, or a pregnancy ultrasound at the end of the pregnancy to help establish the size and position of her baby.
The hospital discharge summary states the indications for her emergency (class 1) Caesarean section as being a previous Caesarean section, high presenting part, uterine rupture, non-reassuring FHR trace, inadequate pelvimetry – clinical and uterine anomaly Bandl’s ring. If the three of these indications indicating her baby was too big for her pelvis (high presenting part, inadequate pelvimetry and Bandl’s ring) had been acted on earlier than was the case she would have had an earlier Caesarean section and uterine rupture would have been avoided.
I am confident I would have recognised in advanced pregnancy that there would most likely be cephalopelvic disproportion (baby too big for the birth canal) in labour, and so increased the risk of uterine rupture. I would have arranged a CT pelvimetry to check the size and shape of her pelvis and a pregnancy ultrasound to help establish the size and position of her baby. With this information and (if any doubt) with the baby’s head being high, her cervix being unfavourable and her being overdue, I would have recommended an elective Caesarean section and not a VBAC attempt. By avoiding labour she would not have had a ruptured uterus and the associated considerable risk to her wellbeing and her baby’s wellbeing and the lower abdominal pain she is now experiencing.
In February 2014 at 40-weeks and six-days pregnancy, she went into labour at home. She had not been advised to go to the hospital for assessment when labour started. This is not in accord with RANZCOG guidelines.
Four hours after the onset of contractions, she became aware of niggly discomfort over the scar, as well as the contractions. She went to the hospital for assessment. She was assessed by the midwife and the baby monitored. The midwife commented her cervix was one to two centimetres dilated and the baby’s head was very high. She was told her baby was in an occipito-posterior position. The baby’s head being so high at 40 weeks and six days was a concern that there may be cephalopelvic disproportion problem looming, but this was not commented on. That her scar discomfort was not taken more seriously is concerning.
She was sent home by the midwife and told to wait at home until she had spontaneous rupture of membranes. With her history of a Caesarean section, I find this decision to send her home, where there could be no monitoring of her or her baby’s wellbeing, very concerning. This is not consistent with best practice. As well, it should not have been the midwife but the obstetric registrar who assessed and made management decisions. She has no recollection of any doctor seeing her until there was foetal distress (much later).
She had spontaneous rupture of membranes at home and with it the onset of more regular and stronger contractions as well as a stabbing pain over her scar. She returned to the hospital where she was assessed. She was told her cervix was now four to five centimetres dilated, but the baby’s head was still high. There was monitoring of her and her baby and it was concluded by the midwife that all was well.
The aetiology of the scar region pain is unclear. It was not the contraction pain. It may be related to stretching of scar tissue in the lower abdominal wall from the previous Caesarean section, but that it indicated early dehiscence of the Caesarean section scar cannot be dismissed. This can happen without the baby’s wellbeing or the maternal wellbeing being affected. Indeed, there can be silent dehiscence of the scar (no pain) in labour and so any woman who has had a successful VBAC needs to have the integrity of her scar checked by an internal examination after delivery.
I suspect the midwife thought if the baby is ok and the woman is ok then the scar is ok. But we still have the concern about cephalopelvic disproportion with the baby’s head being so high at four to five centimetres cervical dilatation. The patient asked for a Caesarean section. I would have been arranging a Caesarean section if she was my patient. In contrast, the midwife arranged an epidural block for the pain and told the patient “you can do it”.
The patient said the epidural block helped for about two hours. She said she then had contraction pain again and another severe pain on the left side of her abdomen. This could be related to a patchy block but with there being two different types of pain is concerning and may indicate the uterine scar tearing.
Three hours later, “I felt weird cramping in my stomach and looked down to blood that started coming out fast. They said it was ok as it was mixed with waters and they said it was just mucous, even though it was bright red.” She said, from monitoring her and her baby, the midwife concluded all was well and her repeated request for a Caesarean section was dismissed.
She said “the pain kept getting worse all over my left side. It was excruciating so they tried topping the EPI up a couple of times with no luck.” Both the bleeding and the constant pain raise concern about the integrity of the uterus scar. The midwife should have arranged for the obstetric registrar to assess.
With the epidural not working, she was increasingly aware of a severe “totally different pain to the contractions” as well as the contraction pain. She had another internal examination by the midwife and she was told her cervix was seven centimetres dilated. Her baby’s head was very high and now to the right of her pelvis. She said the midwife encouraged her to push. In my opinion, she should have been arranging an urgent Caesarean section.
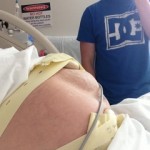
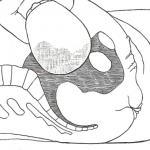
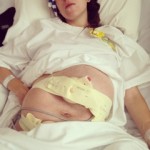 She said her abdomen then took on an unusual shape with a lump on the lower right side and another lump on the upper left side. She said it looked like a figure of eight. See her photos adjacent. It was described to her and has written in the discharge notes as a Bandl’s ring. But no action to do a Caesarean section was taken.
She said her abdomen then took on an unusual shape with a lump on the lower right side and another lump on the upper left side. She said it looked like a figure of eight. See her photos adjacent. It was described to her and has written in the discharge notes as a Bandl’s ring. But no action to do a Caesarean section was taken.
Pathologic retraction ring of Bandl is the result of obstructed labour with marked thinning and ballooning of the lower uterine segment and thickening of the thicker segment. It signifies impending rupture of the lower uterine segment. It is not seen today because of modern obstetric care. So I was shocked when the patient told me about this and I read it in the hospital’s discharge summary. She needed an urgent Caesarean section, but this was not arranged. Instead, it was decided by the midwife she should have spinal block as the epidural was not working.
I have personally never encountered a patient with a pathologic retraction ring of Bandl. In a 1976 obstetric textbook, Williams Obstetrics (by Professor Pritchard and Professor MacDonald), it states it is “rarely seen today, when prolonged and obstructed labours are no longer combatable with good obstetric practice”. In another textbook, Practical Obstetric Problems (by Professor Ian McDonald) of 1974, it states “Rupture is now imminent. The combination of Bandl’s ring rising appreciably within 20 minutes or so together with the threat of tonic contractions indicates the immediate need for delivering the patient by the simplest and therefore safest possible method before uterine rupture actually occurs… If the child is still alive, Caesarean section is the only reasonable treatment.” The question is if there was a pathologic retraction ring of Bandl how was this allowed to happen in Sydney in 2014? If a pathologic retraction ring of Bandl was diagnosed why was not an immediate Caesarean section arranged? It was over two hours between the diagnosis of Bandl’s ring and the eventual decision for her to have a Caesarean section.
She told me with the spinal anaesthetic working “on one side” she said, “I fell asleep for around 10minutes”. She said I woke to “them rushing in saying the baby wasn’t happy. Her heart rate was dipping very low (20 bpm), even between contractions. Tried rolling over but wasn’t helping. The pain in my stomach became constant again and I felt like I was tearing from inside out. The spinal did nothing and I was left in agony all over my entire body again.”
About one hour after her uterus developed the unusual Bandl ring shape, with the patient in severe constant pain (very suggestive of a ruptured uterus) and with an abnormal foetal heart rate pattern (foetal distress in this context is also very suggestive of a ruptured uterus) it was decided to sample her baby’s scalp blood to assess her baby’s wellbeing. The obstetric medical team were now involved in her care, but the decision making was no more sensible. Why did they not decide on an urgent Category 1 Caesarean section rather than a foetal scalp blood pH check?
She said the “head doctor” then came in and asked, “Why is this woman not in theatre?” Thank goodness! “Next thing paperwork had my scribble on it giving them permission for a hysterectomy.” Finally, the Caesarean section decision was made! But it should have been made hours earlier!
She was found to have a ruptured uterus. She said it took over four hours to do the Caesarean section and repair the damage from the uterine rupture. She was told she had considerable blood loss and was given a blood transfusion.
 Her baby was resuscitated in the operating theatre and then taken to the special care baby unit. Her discharge summary said her baby had ‘abnormal blood gases’, suggesting foetal asphyxia (her baby not getting enough oxygen). Her baby has made a full recovery. Her baby had a birth weight of 3.7 kilograms.
Her baby was resuscitated in the operating theatre and then taken to the special care baby unit. Her discharge summary said her baby had ‘abnormal blood gases’, suggesting foetal asphyxia (her baby not getting enough oxygen). Her baby has made a full recovery. Her baby had a birth weight of 3.7 kilograms.
While the hospital discharge summary says that she had been debriefed postnatally, she said to me this had not happened and she has never been given a full explanation of what had happened. Hence, she saw me eight months later.
I suggested the ongoing pain was likely due to scar tissue and possibly adhesions that had formed with healing. We talked about management of her pain. She said to me “Because of this ongoing pain I wish they had done a hysterectomy”. She is only 23 years old! I felt so sad for her. She also asked about another pregnancy. I told her about the increased risk of uterine rupture in another pregnancy.
This tragedy could have been avoided and never had to happen if she had been given good quality obstetric care.
Also see: VBAC – Risks and management

