It is not unusual for a patient to ask: “Is the umbilical cord around my baby’s neck?” The reason for the question is the patient is anxious about this and is concerned the umbilical cord being around baby’s neck (nuchal cord) will adversely affect baby’s wellbeing....
Labour and Delivery
Braxton Hicks contractions and labour pains
Braxton Hicks contractions Braxton Hicks contractions are named after the English doctor John Braxton Hicks who first described them in 1872. He reported many women felt contractions without being near confinement. He said this process was usually painless, but caused...
Supporting your partner in labour
As the husband/partner you have a very important role in supporting your wife/partner during labour and childbirth. There is huge excitement and anticipation that you both have for meeting your new baby. But as well there is anxiety and indeed even fear. Your...
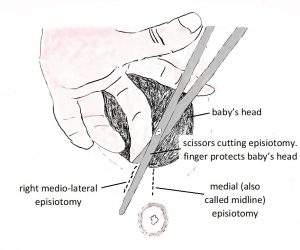
Will I need an episiotomy?
On Friday I had four deliveries. In the afternoon at Norwest Hospital a patient in her first pregnancy had a normal delivery with an intact perineum. That evening at the San Hospital a patient in her first pregnancy had a normal delivery but needed an episiotomy. A...
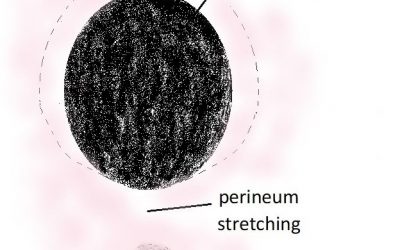
Avoiding significant perineal trauma with childbirth
Rosemarie saw me for management of her first pregnancy. The pregnancy was uneventful. She was admitted to hospital in spontaneous labour when she was 39 weeks gestation. She had an epidural for pain relief in labour. In second stage labour there was slow progress with...
Pain relief in labour
There are a variety of options for pain relief in labour. Which one a woman chooses depends on variables such as her background wishes, expectations, labour and childbirth history, her fears, how quickly her labour progresses and developments in the labour. There is...
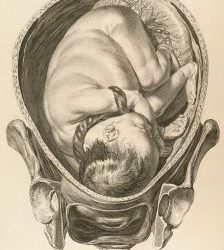
Is my baby in the right position?
This is a very common question to be asked by a patient in advance pregnancy. Usually, when a patient asks me this question she is asking if her baby is in an occipito-anterior position. Occipito-anterior is when the back of baby’s head (the occiput) is toward the...
Labour and Delivery
What is labour? First stage labour is defined as regular coordinated contractions that cause your cervix to dilate. The onset of labour is when your contractions cause this to happen. There may be increased uterine activity in the days or even weeks before true labour...
Induction of Labour
What is induction of labour? Induction of labour is a procedure done to end a pregnancy after 20 completed weeks with the goal being a normal vaginal delivery. When is induction of labour considered? Induction is considered when there are complications of pregnancy...
Rupture of Membranes
I think my waters have gone! Rupture of membranes (ROM) or “waters have gone” refers to the leaking of amniotic fluid (‘liquor’) from the amniotic sac around your baby because of a hole that develops in the amniotic membrane. It is a normal phenomenon during labour....
Vacuum and Forceps
When are vacuum cups and forceps used when delivering a baby? For an operative vaginal delivery and sometimes with a Caesarean section delivery. Will I need an operative vaginal delivery? Hopefully not. Only about 12% of my patients need operative vaginal deliveries....
Caesarean section Delivery
Will I need a Caesarean section? A Caesarean section is an abdominal operation to deliver your baby. It is either an emergency or elective operation. An emergency Caesarean section is done when there is an urgent complication in pregnancy or labour which significantly...
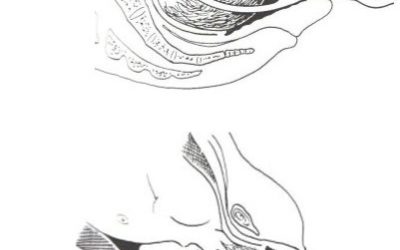
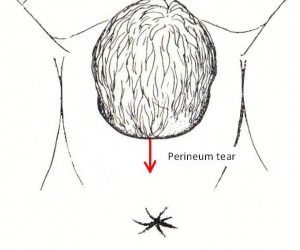
Perineal Tearing at Delivery
Perineal tearing The goal with a vaginal delivery is an intact perineum. This does not always happen. There can be tearing, the commonest area of tearing is the perineum. Hopefully it is only minor tearing. Sometimes an episiotomy is needed. This could be to avoid a...
Birth plan – Do I need one?
Some of my friends have said I need a birth plan. Is this necessary? Answer: No – this is not necessary. The birth plan concept is more relevant for pregnant women going through the public system to have their baby where there is no personalised care and the staff...
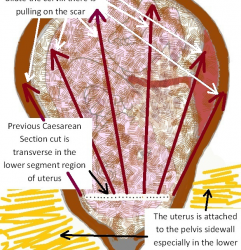
VBAC – Risks and management
This article is for my patients who have had a Caesarean section and are considering attempting a VBAC delivery this time. It’s purpose is to give you comprehensive information to help you to make your decision whether or not to attempt a VBAC. The contents of this...
Book an appointment now
- Monday all day 9.00am to 4.30pm
- Tuesday all day 9.00am to 4.30pm
- Wednesday all day 9.00am to 4.30pm
- Thursday morning 9.00am to 12.30pm
- Thursday alternate afternoons 2.00pm to 4.30pm
- Friday alternate mornings 9.00am to 1.00pm
- Friday afternoon 2.00pm to 4.30pm
- Saturday mornings 9.30am to 12.00 midday*
*Saturday morning appointments are not available for initial antenatal visit.